Reduced quality of life
Interference and limitation in daily activities
Sleep disturbances
Economic cost
What is allergy?1
Allergy is a hypersensitivity or exaggerated response of the immune system to elements in our environment (pollens, dust mites or food, for example) that pose no threat to us. This immune imbalance is associated with a series of inflammatory reactions in different organs and mucous membranes of the body, which give rise to the different symptoms and signs of allergic diseases. There are immediate and delayed hypersensitivity reactions, with immediate reactions (mediated by the IgE antibody) being the most common.
Within the different existing allergic pathologies, we speak of dermatitis when the inflammation affects the skin, conjunctivitis if it occurs in the conjunctiva of the eye, rhinitis when it affects the nasal mucosa or asthma if the inflammation affects the bronchi.
What causes allergies?2
Agents that cause allergic diseases are called allergens. These can be defined as harmless substances that induce hypersensitivity reactions in susceptible persons.
They cause diseases through inhalation and subsequent contact with the respiratory tract (asthma, rhinitis) and/or the conjunctiva of the eye (conjunctivitis). The most common aeroallergens are pollens, fungal spores, dust mites and domestic animals.
They produce immediate reactions to their consumption, with the appearance of digestive, respiratory and/or skin symptoms. The most common in children are milk and egg proteins, while in adults fruit and shellfish predominate. Allergy to parasites that contaminate food, such as allergy to Anisakis simplex larvae in fish, is also considered to be of food origin.
They produce skin reactions in contact with the skin over a more or less prolonged period of time, which manifest themselves in the form of eczema or dermatitis. The most common contact allergens are metals (especially nickel) and some topical medicines.
These are medicines, latex, venom from hymenoptera (bees and wasps).
What types of allergy tests are there and how are they how are they performed? 3
In clinical practice, the etiological diagnosis of allergy is made by means of the clinical history complemented by the allergological study. For the allergological study, skin tests and in vitro specific IgE determinations showing sensitization, i.e. the presence of specific IgE against the aeroallergen, are available.
Several types of skin test can be performed, depending on the allergic disease being treated and the type of allergic reaction (immediate or delayed) suspected.
Prick test
The most widely used and performed allergy test. It is used to investigate allergy mediated by immunoglobulin E (IgE), also known as immediate hypersensitivity reaction.
To carry out the test, a drop of the allergen extract to be tested is placed on the front of the forearm and a slight puncture is made with a lancet through the drop of extract and the outermost layer of skin (epidermis). The response is obtained within a few minutes.
A variant of this test is the prick test: it consists of pricking the substance in its natural state (for example, a fruit) with the lancet and then pricking the skin with the same lancet.
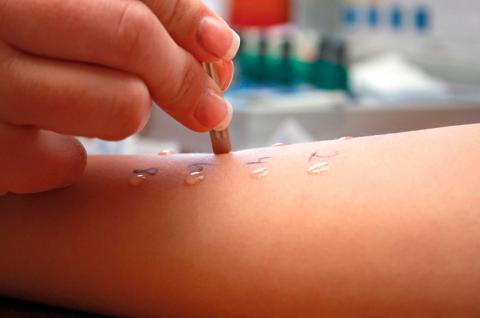
Skin test
It is the most important in the investigation of certain allergic skin diseases, such as allergic contact dermatitis (allergic eczema) or certain drug reactions.
The substance is usually mixed with Vaseline and placed in contact with the skin using special dressings or polyethylene patches, keeping the substance in contact with the skin for a few days. After 48 hours, the patches are removed and the reaction is checked. At 96 hours, without having washed the area, a final reading is taken.
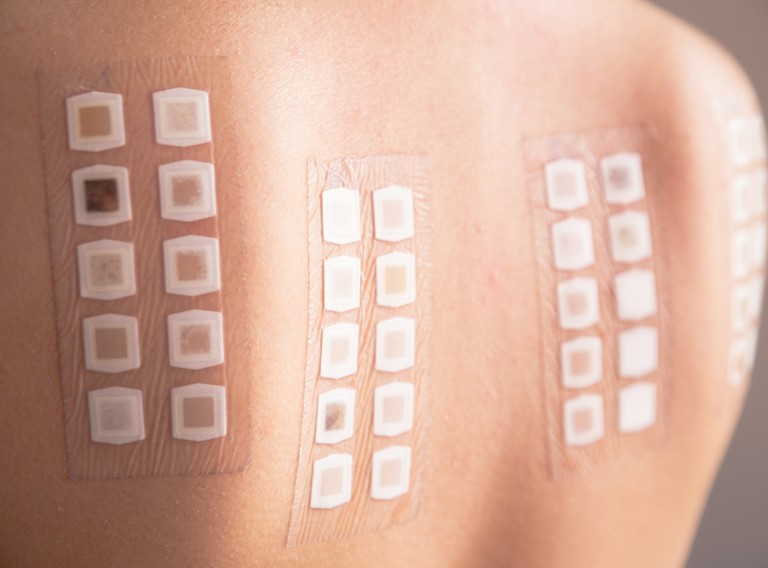
Intradermal test
More expensive and laborious test. For some allergens (hymenoptera venom, medicines or people with low sensitivity), the prick test is not enough. In these cases, intradermal tests are recommended (they are more sensitive).
It consists of the direct injection of the extract deeper into the second layer of the patient's skin (dermis), and the reading is taken after 15-20 minutes. It is also useful for investigating delayed-type hypersensitivity, and a reading should be taken at 24, 48 and 96 hours.
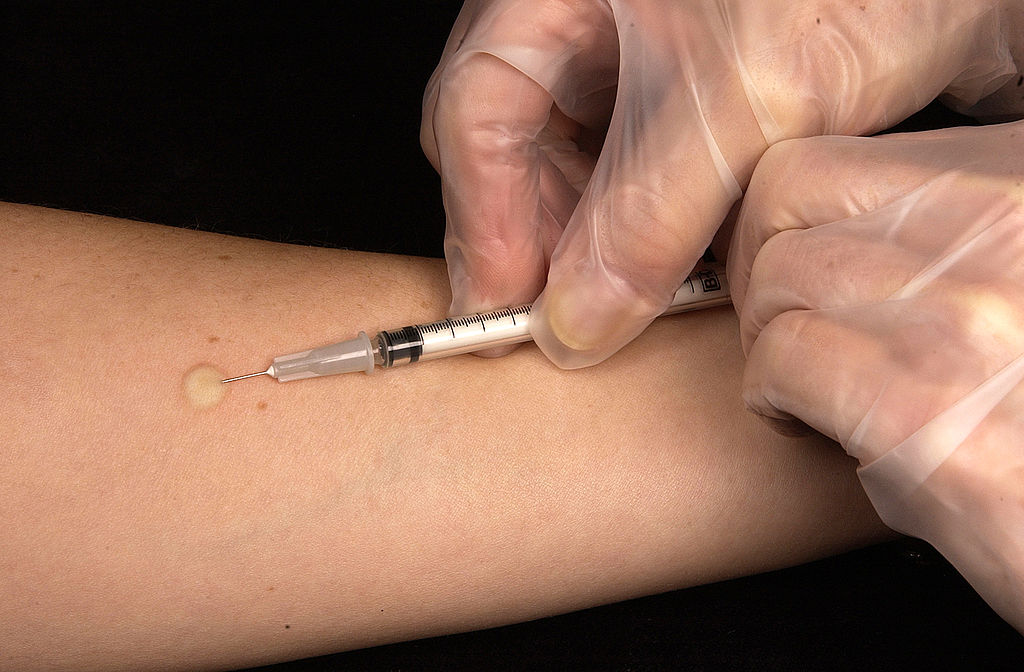
1. Chivato Pérez T. ¿Qué es la alergia? ¿Qué estudia la Alergología? En: José Manuel Zubeldia, Mª Luisa Baeza, Ignacio Jáuregui, Carlos J. Senent. BBVA Foundation book on allergic diseases. 1st ed. Bilbao: Editorial Nerea, S.A.; 2012. p. 21-30.
2. SEAIC: Sociedad Española de Alergología e Inmunología Clínica (cited on October 10, 2010). Available at: https://
www.seaic.org/pacientes/conozca-sus-causas
3. Parra Arrondo A. The skin tests. En: José Manuel Zubeldia, Mª Luisa Baeza, Ignacio Jáuregui, Carlos J. Senent. Libro de las enfermedades alergénicas de la fundación BBVA. 2.ª ed. Bilbao: Editorial Nerea, S.A.; 2012. p. 365-370.







